What are the chances of another pandemic worse than COVID?Qual a chance de outra pandemia pior que a COVID?
The world still remembers the profound impact of COVID-19 on our daily lives. While we have moved forward, many experts now question if we are truly prepared for a future health crisis that could be even more severe. Concerns reached a new peak following the 2026 viral sample theft incident in São Paulo. This alarming event highlighted significant vulnerabilities in how we secure dangerous pathogens. It serves as a stark reminder that our collective safety depends on strict oversight and international cooperation.
3/27/202612 min read


Maintaining global health requires us to stay vigilant against emerging biological threats. We must analyze these risks to build a more resilient infrastructure. By understanding the lessons from recent history, we can better protect our communities from the next potential pandemic.
Key Takeaways
The 2026 São Paulo viral theft raised urgent questions about laboratory security.
Experts believe that future health threats could surpass the severity of previous outbreaks.
Strengthening international cooperation is essential for effective disease prevention.
Public awareness plays a critical role in supporting global health initiatives.
Proactive monitoring of pathogens helps mitigate the risk of a widespread pandemic.
The 2026 São Paulo Incident: A Case Study in Biosecurity
The 2026 São Paulo incident is a stark reminder of the vulnerabilities in our current biosecurity measures. This event highlighted the potential risks associated with the handling and storage of viral samples in research facilities.
In São Paulo, a significant breach occurred, leading to the theft of viral samples from a laboratory. This incident not only raised concerns about the security protocols in place but also about the potential consequences of such a breach.
The Theft of Viral Samples
The theft of viral samples is a serious incident that can have far-reaching consequences. In the case of the São Paulo incident, the stolen samples included potentially dangerous pathogens that could be used for malicious purposes.
The incident underscored the need for robust security measures to prevent unauthorized access to such materials. Laboratories handling viral samples must implement stringent controls to mitigate the risk of theft.
Immediate Security Protocols and Failures
Upon discovery of the theft, immediate action was taken to assess the security protocols in place at the laboratory. The investigation revealed several lapses in the security measures, including inadequate surveillance and insufficient personnel training.
The São Paulo incident serves as a critical reminder of the importance of regularly reviewing and updating security protocols to prevent such breaches in the future.
Assessing the Global Risk of a New Pandemia
Assessing the risk of a new pandemic requires a multifaceted approach that considers various factors, including pathogen evolution and zoonotic spillover. The global community must be vigilant and proactive in understanding these risks to mitigate the impact of potential future outbreaks.
Pathogen Evolution and Zoonotic Spillover
Pathogen evolution is a critical factor in the emergence of new pandemics. As pathogens evolve, they can become more virulent or transmissible, posing significant risks to human health. Zoonotic spillover, the process by which pathogens jump from animals to humans, is another key mechanism behind the emergence of new infectious diseases.
The risk of zoonotic spillover is heightened by factors such as deforestation, climate change, and increased human-animal contact. Understanding these dynamics is crucial for predicting and preventing future pandemics.
The Role of Laboratory Research in Modern Science
Laboratory research plays a vital role in understanding and mitigating pandemic risks. Through the study of pathogens in controlled environments, scientists can gain insights into their behavior, evolution, and potential for transmission to humans.
Moreover, laboratory research is essential for the development of diagnostic tools, vaccines, and treatments. By advancing our knowledge of pathogens and improving our ability to counter them, laboratory research is a cornerstone of pandemic preparedness.
Lessons Learned from the COVID-19 Crisis
The COVID-19 pandemic has left an indelible mark on global health infrastructure, prompting a thorough examination of our preparedness and response mechanisms. As we reflect on the lessons learned, it becomes clear that the pandemic exposed both the resilience and vulnerabilities of global health systems.
The response to COVID-19 was multifaceted, with various stakeholders playing critical roles. Governments, healthcare professionals, and the public each contributed to the efforts to mitigate the pandemic's impact. However, the effectiveness of these efforts varied widely across different regions and communities.
What We Got Right and Where We Failed
One of the significant achievements during the COVID-19 pandemic was the rapid development and distribution of vaccines. This was made possible by unprecedented global collaboration among scientists, governments, and pharmaceutical companies. Vaccine development was accelerated through the use of new technologies and streamlined regulatory processes, allowing for the deployment of effective vaccines in record time.
Despite these successes, there were significant failures in the global response. Early warning systems were not robust enough to detect and respond to the pandemic in its initial stages, leading to delays in implementing critical public health measures. Additionally, the lack of standardized protocols for data sharing and communication hindered the coordination of a unified global response.
The Fragility of Global Supply Chains
The COVID-19 pandemic highlighted the fragility of global supply chains, particularly in the healthcare sector. The surge in demand for personal protective equipment (PPE), ventilators, and other critical medical supplies exposed weaknesses in global production and distribution networks.
The reliance on just-in-time manufacturing and global sourcing led to shortages and delays in the delivery of essential supplies. This not only affected the ability of healthcare systems to respond to the pandemic but also had broader economic implications, as supply chain disruptions rippled through various industries.
To mitigate these risks, there is a need to diversify supply chains and build more resilient production and distribution networks. This could involve strategies such as localizing production for critical supplies, enhancing inventory management practices, and developing more flexible and adaptable supply chain architectures.
In conclusion, the COVID-19 pandemic has provided valuable lessons for improving global health security. By understanding what worked well and where the response fell short, we can develop more effective strategies for preparing for and responding to future pandemics.
The Reality of Pathogens Outside Controlled Environments
The risk of pathogens escaping controlled environments is a pressing concern in the scientific community. Laboratories handling dangerous pathogens must adhere to strict biosafety protocols to prevent accidents.
Biosafety levels are critical in determining the level of containment required for handling different types of pathogens. Facilities working with highly dangerous pathogens are required to have advanced safety measures in place.
Understanding Biosafety Levels and Containment
Biosafety levels are categorized into four tiers, with level 4 being the most secure. BSL-4 laboratories are designed to handle the most dangerous and exotic pathogens.
Containment procedures are put in place to prevent the escape of pathogens. This includes the use of personal protective equipment (PPE), secure laboratory design, and strict protocols for handling and disposing of pathogens.

The Human Factor in Laboratory Security
Despite advanced safety measures, the human factor remains a significant risk in laboratory security. Human error can lead to accidents and the potential release of pathogens.
Training and adherence to protocols are crucial in minimizing the risk of human error. Laboratories must invest in comprehensive training programs for their staff to ensure they understand and follow safety procedures.
Moreover, a culture of safety within the laboratory is essential. This includes regular audits, feedback mechanisms, and a clear understanding of the importance of biosafety among all staff members.
Technological Advancements in Pandemic Surveillance
The field of pandemic surveillance is witnessing a revolution thanks to cutting-edge technology. This transformation is crucial in the early detection and management of outbreaks, potentially saving countless lives and preventing widespread economic disruption.
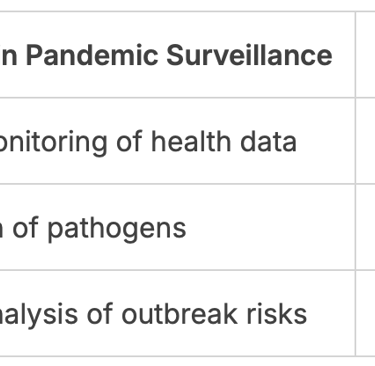
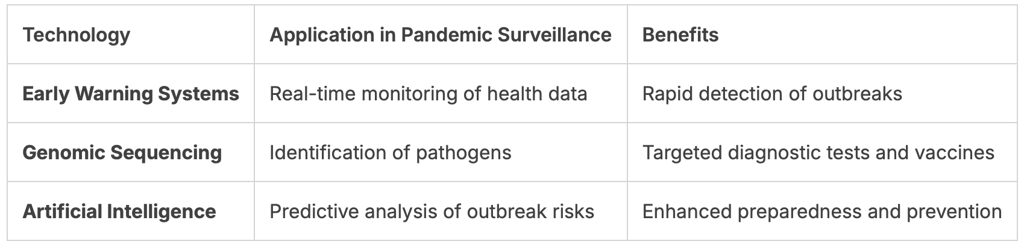
Early Warning Systems and Genomic Sequencing
One of the key advancements in pandemic surveillance is the development of early warning systems. These systems leverage real-time data from various sources, including social media, healthcare providers, and environmental sensors, to detect anomalies that could indicate the onset of an outbreak. Genomic sequencing plays a vital role in this process by enabling the rapid identification of pathogens.
Genomic sequencing technologies have become increasingly sophisticated, allowing for faster and more accurate identification of viral and bacterial strains. This capability is essential for understanding the evolution of pathogens and for developing targeted diagnostic tests and vaccines.
Artificial Intelligence in Predicting Outbreaks
Artificial intelligence (AI) is being increasingly utilized to predict potential outbreaks. AI algorithms can analyze vast amounts of data from diverse sources, identifying patterns that may elude human analysts. This predictive capability can significantly enhance the effectiveness of early warning systems.
The integration of AI in pandemic surveillance also facilitates the analysis of genomic data, helping to identify potential hotspots for disease emergence. By understanding these risks, public health officials can implement targeted interventions to prevent outbreaks.

The Psychological Impact of Potential Future Threats
Living with the threat of another pandemic can have profound effects on mental health worldwide. The constant fear of a potential outbreak can lead to increased levels of anxiety, stress, and depression among the general public.
The psychological impact is not limited to the general population; it also affects healthcare workers, policymakers, and other stakeholders who are directly involved in managing and mitigating pandemic risks. The need for effective strategies to manage public anxiety and combat misinformation is more pressing than ever.
Managing Public Anxiety
Managing public anxiety requires a multi-faceted approach that includes transparent communication, public education, and community engagement. Authorities must work to build trust by providing accurate and timely information about potential threats and the measures being taken to mitigate them.
"Trust is the glue of life. It's the most essential ingredient in effective communication. It's the foundational principle that holds all relationships." - Stephen Covey
Public education campaigns can play a crucial role in preparing the public for potential future pandemics by disseminating information on preventive measures, symptoms, and what to do in case of an outbreak.
Combating Misinformation
Combating misinformation is another critical aspect of managing the psychological impact of potential future threats. Misinformation can spread rapidly through social media and other channels, exacerbating public anxiety and leading to inappropriate behaviors.
Implementing fact-checking mechanisms
Promoting credible sources of information
Encouraging social media platforms to take responsibility for the content they host
Technological solutions, such as AI-powered fact-checking tools, can also be leveraged to identify and counter misinformation.
Building Resilience
Building resilience in a post-COVID world involves not just mitigating the immediate psychological impacts but also fostering long-term mental health and well-being. This can be achieved through community-based initiatives, mental health support services, and policies that promote overall well-being.


By adopting a comprehensive approach to managing public anxiety, combating misinformation, and building resilience, we can better prepare for and respond to future pandemics.


International Cooperation and Global Health Governance
Global health security is inextricably linked to international cooperation and the strength of global health governance frameworks. The recent pandemic has shown that health crises can have far-reaching consequences, affecting economies, societies, and political stability worldwide. Therefore, it is crucial to examine the mechanisms that can enhance global health governance and foster international cooperation.
The Role of the World Health Organization
The World Health Organization (WHO) plays a pivotal role in global health governance. It coordinates international health responses, provides technical guidance, and monitors health trends worldwide. The WHO's ability to respond effectively to health crises depends on the cooperation of its member states and the robustness of its governance structures.
One of the WHO's key functions is to provide a platform for countries to share information, coordinate responses, and develop common standards for health care. This includes setting guidelines for biosafety and biosecurity, which are critical in preventing the misuse of biological agents.
Standardizing Biosafety Regulations Across Borders
Standardizing biosafety regulations is essential for preventing biological threats. Different countries have varying levels of biosafety standards, which can create vulnerabilities in the global health security framework. Harmonizing these regulations can help ensure that laboratories and research facilities worldwide adhere to best practices, reducing the risk of accidents or intentional releases of harmful pathogens.
The process of standardization involves international collaboration and agreement on minimum safety standards. This can be facilitated through the WHO and other global health authorities, which can provide technical assistance and support to countries in need.
Are We Truly Prepared for a Worse Scenario?
The COVID-19 pandemic has left an indelible mark on global health security, raising critical questions about preparedness for future pandemics. As we reflect on the lessons learned and the steps taken since the onset of COVID-19, it is crucial to evaluate our current state of readiness for a potentially worse scenario.


Evaluating Current Healthcare Infrastructure
A critical aspect of pandemic preparedness is the robustness of our healthcare infrastructure. This includes not only the physical facilities and equipment but also the personnel and systems in place to respond to a health crisis. Investments in healthcare infrastructure have been made in various parts of the world, but the question remains whether these investments are sufficient to handle a pandemic worse than COVID-19.
The capacity of hospitals, the availability of medical supplies, and the ability to scale up testing and contact tracing are all crucial components. For instance, during the COVID-19 pandemic, many countries faced challenges in securing personal protective equipment (PPE) and ventilators. Have we adequately addressed these shortages?
Have hospital capacities been expanded or made more flexible?
Are there robust supply chains in place for critical medical equipment?
Have healthcare workers received the necessary training to handle a more severe pandemic?
The Gap Between Policy and Practice
While policies and guidelines for pandemic preparedness have been developed and disseminated, the implementation of these policies on the ground is often where the real challenge lies. The gap between policy and practice can be significant, and it is here that the true test of preparedness is found.
"The biggest challenge is not the policy itself, but ensuring that it is effectively implemented and that all stakeholders are held accountable."
Effective pandemic preparedness requires not just well-crafted policies but also the political will and operational capacity to implement them. This includes ensuring that local communities are engaged and that there is a clear understanding of the roles and responsibilities of different actors.
To bridge this gap, it is essential to:
Enhance coordination between different levels of government and healthcare providers.
Invest in training and capacity-building for healthcare workers.
Engage communities in preparedness efforts to build trust and compliance.
Conclusion
As the world continues to navigate the complexities of global health, the threat of another pandemic remains a pressing concern. The discussions around the 2026 São Paulo incident, global risk assessment, and lessons learned from the COVID-19 crisis underscore the need for robust pandemic preparedness measures.
Effective biosecurity protocols, coupled with advancements in technological surveillance and international cooperation, are crucial in mitigating the risks associated with emerging pathogens. The role of global health governance, led by organizations like the World Health Organization, is vital in standardizing biosafety regulations and ensuring a unified response to potential outbreaks.
To be truly prepared for a worse scenario, it's essential to bridge the gap between policy and practice, evaluating and strengthening current healthcare infrastructure. By doing so, we can build resilience in a post-COVID world and reduce the psychological impact of potential future threats.
Ultimately, the path forward requires sustained vigilance, improved preparedness, and a commitment to global cooperation in the realms of pandemic preparedness, global health, and biosecurity.
FAQ
Is there a significant chance of another pandemic emerging that is worse than COVID-19?
While we hope for the best, experts and organizations like the World Health Organization (WHO) warn that the risk is real. The 2026 viral sample theft in São Paulo served as a major wake-up call, demonstrating that biosecurity breaches can happen even in high-security environments. When you combine potential lab accidents with natural zoonotic spillover and pathogen evolution, the necessity for constant vigilance and global preparedness becomes very clear.
What exactly happened during the 2026 São Paulo incident?
The 2026 incident involved the high-profile theft of viral samples from a research facility in São Paulo, Brazil. This event exposed critical vulnerabilities in biosecurity protocols and highlighted how the "human factor"—such as internal security lapses or social engineering—can undermine even the most advanced technical safeguards. It has since become a primary case study for laboratories worldwide to improve their containment strategies.
What are Biosafety Levels (BSL), and why do they matter?
Biosafety Levels, ranging from BSL-1 to BSL-4, are a series of protections centered on laboratory settings. They are designed to protect workers, the environment, and the public. For instance, BSL-4 labs handle the most dangerous pathogens, such as Ebola or Marburg virus, using airtight enclosures and specialized ventilation. Ensuring these levels are strictly maintained is vital to preventing the accidental release of infectious agents into the community.
How is Artificial Intelligence helping us predict future outbreaks?
Artificial Intelligence (AI) is a game-changer for pandemic surveillance. By analyzing massive datasets—from social media trends to climate change patterns—AI can identify potential "hotspots" for outbreaks before they spiral out of control. When paired with genomic sequencing, researchers can quickly map the DNA or RNA of a new virus, allowing institutions like the CDC and GISAID to share life-saving data across borders in real-time.
Why did global supply chains struggle so much during the COVID-19 crisis?
The COVID-19 pandemic revealed that our global supply chains were "just-in-time" rather than "just-in-case." This led to a dangerous fragility in the distribution of Personal Protective Equipment (PPE), semiconductors, and essential medicines. Today, there is a stronger focus on diversifying manufacturing and building local stockpiles to ensure that a future crisis doesn't paralyze international trade and healthcare delivery.
How can we manage public anxiety and misinformation regarding future health threats?
Transparency is the best tool for building resilience. By providing clear, science-based communication and addressing rumors early, health authorities can reduce the "infodemic" that often accompanies a crisis. Psychological health is just as important as physical health; therefore, community-based support and accurate reporting are essential to keep the public informed and calm in a post-COVID world.
What is the role of the World Health Organization in preventing the next pandemic?
The WHO acts as the central coordinator for Global Health Governance. Their role includes standardizing biosafety regulations across borders and facilitating international cooperation through initiatives like the Pandemic Accord. Because viruses do not respect national boundaries, the WHO ensures that countries share information and resources to stop a local outbreak from becoming a global catastrophe.
Are our current healthcare infrastructures truly prepared for a worse-case scenario?
While we have made incredible technological leaps, there is still a noticeable gap between policy and practice. Many healthcare systems are still recovering from the exhaustion of previous years. Real preparedness requires more than just high-tech surveillance; it requires robust funding for frontline workers, modernized hospital facilities, and a commitment to international cooperation that transcends political differences.
Contact
Contact us for questions or suggestions.
© 2025. All rights reserved.
suportedoisb@gmail.com
